Monday November 16, 2020 | VICTORIA, BC [Updated 10:45 pm]
by Mary P Brooke, B.Sc., editor | Island Social Trends
Keeping with the current trend, today’s COVID-19 case numbers were high.
Provincial Health Officer Dr Bonnie Henry said today in her usual Monday media briefing that over the weekend and into today (a three-day count by the BC Centre for Disease Control (BC CDC), that there are 1,959 new cases.
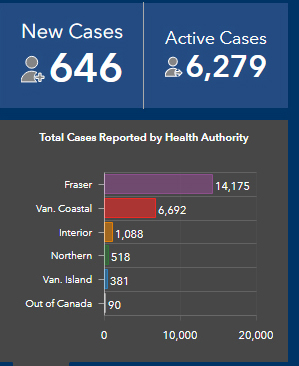
That’s an average of 653 per day, which is even higher than the previous peak of 617 seen just ahead of the weekend). The day-by-day count over the last weekend was: 654 (Friday to Saturday, November 14 to 15; 659 (Saturday to Sunday, November 15 to 16); and 646 (Sunday to Monday, November 16 to 17).
Presently 10,928 people are self-isolating due to exposure to known cases of COVID-19. That’s down somewhat from a peak of 12,016 on Friday the 13th.
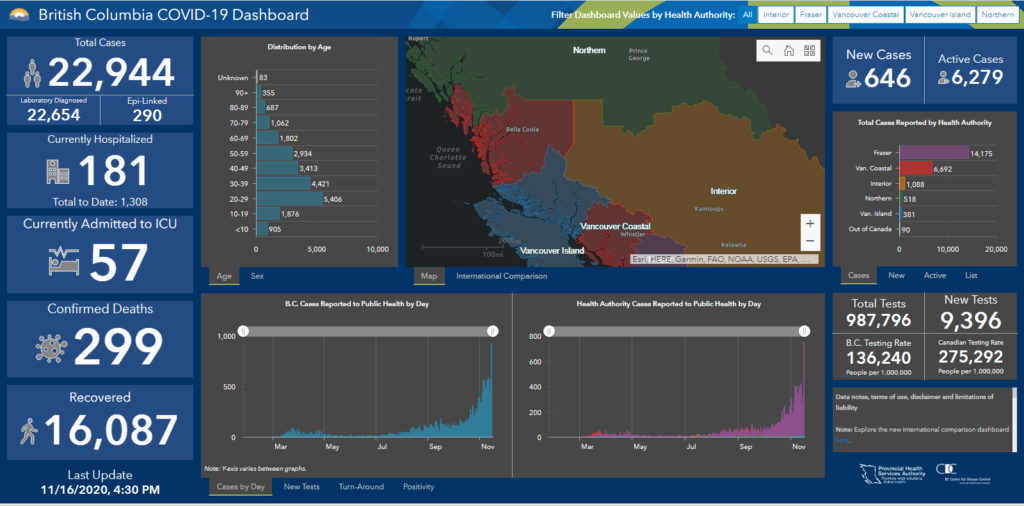
COVID hospitalizations in BC are up, now 181 people (57 in ICU). There have been 1,308 hospitalizations in BC during the pandemic to date. A higher rate of hospitalization of course puts the health-care system on higher alert. It puts additional strain on personnel and procedures, as well as supplies of personal protective equipment (PPE).
Health Minister Adrian Dix today said that 43 pallets of PPE arrived by air cargo this past weekend. That large shipment is being sorted and tested before being distributed to where it’s needed around the province.
Outbreaks:
There have been 11 new health-care outbreaks, bringing the active total to 52 (45 in long-term care and seven in acute care).

Death count up:
There were nine deaths by COVID over the weekend (in the lower mainland and northern BC). That’s the highest death count increase in a long while.
Minister Dix and Dr Henry always offer their condolences to the families and caregivers, particularly as it’s even more difficult to grieve in usual ways during a pandemic where people must ‘stay apart to stay safe’.
Vancouver Island focus:
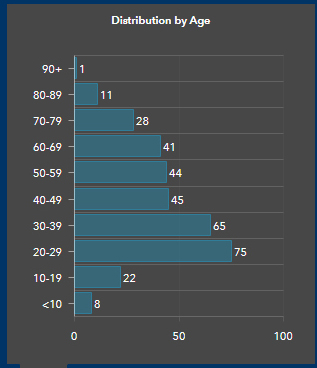
There are 41 new cases on Vancouver Island in today’s three-day report, which is high for the Island Health region (total now 381 cases, of which 99 are active).
There were new-case increases in all age groups, which differs from most previous weeks. Now two people are in hospital in Island Health due to COVID-19 (one in ICU). This indicates more active transmission on the island, harkening back to the first wave in March and April.
The case distribution of 99 active cases by region on Vancouver Island is 30 in the south, 50 central and 19 in the north.
No new deaths on Vancouver Island (tally has been six since September 28).
In the second wave:
BC is clearly in the second wave of COVID-19. Dr Henry asks that people not gather with people, that people stick close to home as much as possible, and not travel (especially to the zones with high rate of infection) unless it’s essential.
“Stay in your communities now,” she said today. “The virus comes with us. Now is not the time for recreational or non-essential travel.” BC’s top doctor also articulated that this is not the time to travel to or from other provinces.
Again, she stressed that people are to use their layers of protection, limit their socializing, and limit their travel.
Cases have developed through transmission at weddings, fitness centers and workplaces. Dr Henry asks each person to consider the consequences of their actions. She would like people to “shrink back to their pandemic bubble” at this point. She says that will help keep surgeries happening and schools continuing to function.
It’s still safe to walk outdoors for recreation outdoors without wearing a mask, Dr Henry said today. Though she did add that in cold winter weather a mask could actually add a level of physical comfort. “Going for a walk with somebody is safe. Keep your distance as much as possible. But walking by somebody is not a high risk situation,” she summarized.

“We should be focusing on those situations where we know this virus is more likely to transmit, and that is indoor settings, particularly where we’re spending more than 15 minutes, face to face with somebody,” said Dr Henry.
She noted hair salons, barber shops and nail salons as “places where we’re spending time with people”.
“We know that masks can be very effective as part of the different things that we have in place that prevent transmission in those settings,” said Dr Henry.
Winter break might come sooner:

Dr Henry said today that she pondered the idea of winter break for public schools coming sooner than normally scheduled.
But she repeats that transmission is lower in schools than in the general community. A longer winter break where families are home in shared closed spaces could add to transmission.
She noted that a high fever is not a common symptom of COVID-19, and that’s the reason why temperature checks are not done in schools.
What about Christmas:

“I don’t know the answer to that yet,” was Dr Henry’s response to Island Social Trends‘ question today about whether people will need to celebrate Christmas at home with only their household members, or whether family and friends from their safe six can be there too.
“What we’re telling people right now — and this is because of what we’re seeing right now — if you’re in Fraser Health and lower mainland Vancouver Coastal region you need to stick to your household bubble only,” said Dr Henry.
“This is thinking back to where we were in April. Those people who are our close contacts, our close household. We put out some definitions of household… it’s different for different people (as to) who our family is. It may be people were related to, or people we’re close to,” she explained.

If people live alone that could be one or two other people who are in their pandemic bubble. For some families who have children who live with both parents that may be two families. “Right now, that is the focus,” Dr Henry said.
She continued: “In the rest of the province we’re starting to see increased transmission in our community. There’s an order about this. You need to stick to your safe six. Your household plus that one set of set of six people that your family is connected to.”
“Right now, we need to think about reducing all of our social gatherings. If it’s not necessary to visit, don’t do it right now. Give it a break, let us get the numbers down. And it’s most important in those areas where we’re seeing a lot of community transmission. But this is spreading around our province and we now know that the season makes it easier for this virus to spread. So all of us need to think about no gathering, but supporting our families and our friends in remote ways and ways that are safe,” was Dr Henry’s final word at this point about Christmas 2020 during the COVID-19 pandemic.

What was not discussed today are the emotional and social impacts of making those choices among families or friends for the special day or season. The short-term agreement to ‘stay apart to stay safe’ could still in many cases have long-term social-emotional impacts. Who ‘wins’ the family lottery and who doesn’t. Who spends that day alone. The mental health aspects of dealing with COVID overall have been well noted already during the pandemic.
Santa’s got it:

Last week Dr Henry said she’s pretty sure that Santa is immune to COVID-19.
That’s the 2020 version of “Yes, Virginia, there is a Santa Claus,” as in reassuring children of all ages about the enduring power of love and hope that is sought and reaffirmed at Christmas time.
Businesses are encouraged to be tough:
Businesses with COVID-safety plans are the best line of defence rather than relying on enforcement, Dr Henry explains. Both customers/clients and employees are expected to follow the COVID-safety plans established by any business or workplace. If people show up without a mask they should be provided with one or told to shop by curbside pickup or online, she said today.
Some good news about vaccines:
Dr Henry said “it’s encouraging news today” regarding word that two vaccines could be available in the first part of 2021. That’s from Pfizer and Moderna. “Very soon within weeks or months,” said Dr Henry about distributing the new vaccines.
But meanwhile, everyone needs to be “doing their bit”, by continuing to follow all COVID-19 public health protocols. This is a tone of cautious optimism.
Even when a vaccine comes there will be distribution challenges. For starters, there’s the shipping and storage temperature requirements. The Pfizer vaccine will require storage at or below minus-70°C while the Moderna vaccine requires ‘only’ minus-20°C — “we have lots of freezers for those,” and that vaccine can therefore be distributed in a number of different ways, said Dr Henry today. Apparently the Moderna vaccine will also last about 25 days longer than the Pfizer vaccine.
Moderna data released today showed that side effects were generally short-lived and there were no significant safety concerns, and no serious COVID cases developed among trial participants who got the vaccine.
Other logistical challenges for the Pfizer vaccine (which Dr Henry described as ‘fussy’) include getting the vaccine from the deep-freeze to distribution locations (remaining cold all the while) and reconstituting the frozen product into dosages. “That means that certain vaccinators will have to deliver that vaccine,” said Dr Henry, making the first clear distinction about how it won’t be ‘one size fits all’ when it comes to vaccine distribution.
She said the vaccine needs “to be licenced for use in Canada and (to determine) for whom it works best — these are other considerations. “And we don’t yet have those details,” she explained.
There will be national standards and an “ethical framework” to follow as to who gets the vaccine first. Frontline and essential workers in health-care and other sectors will be first, of course, as well as people who are already hospitalized with other health challenges, and key workers and leaders in various parts of the country and in communities.
“It’s going to make a difference,” said Dr Henry about the upcoming vaccines. But “it’s not a light switch”. Life won’t go back to pre-COVID. There will still be hand washing. “That will never change,” she declared.
By next fall, perhaps, there could be a vaccine for everyone, said Dr Henry today. “I’m confident that by this time next year we will have vaccine available for everyone in British Columbia,” said Dr Henry in a rather bold statement considering the magnitude of resting one’s hopes on that vision of the future.
Science behind the vaccines:

Both the Pfizer and Moderna vaccines were developed with a strategy to use messenger RNA, which is new approach in terms of vaccine development. This type of vaccine is designed to transform the human body’s own cells into vaccine-making factories. The vaccine instructs human cells to make copies of the spike protein of the coronavirus, stimulating the creation of protective antibodies.
Pfizer claims 90% effectiveness for their vaccine while Moderna claims 94.5% for theirs. Today federal Health Minister Patty Hajdu said this is “good news, but early news”.
The business angle:
A lot about developing vaccines depends on the business angle. Deep-pocket development in return for larger return, or requiring money upfront from governments or other sources.
According to Bloomberg News, Moderna received $955 million from the U.S. Operation Warp Speed program. Pfizer has said it didn’t receive any federal funding to develop its vaccine, though BioNTech got as much as 375 million euros ($444 million) in German government assistance. However, Pfizer has struck a supply agreement with the U.S. worth nearly $2 billion. The U.S. has agreed to pay up to $1.53 billion to purchase supply of the Moderna shot.




