Friday April 17, 2026 | VICTORIA, BC
by Mary P Brooke | Island Social Trends
The drug overdose crisis that was declared a public health emergency in British Columbia is now 10 years in.
People use drugs (by choice or coercion) and are exposed to drugs (sometimes entirely by accident).
The victims of this crisis are young and older. It crosses all socioeconomic levels for education and life circumstance.
4.1 deaths per day:
This week the BC Coroners Service reported that there were 115 unregulated drug-toxicity deaths in February 2026. That equates to about 4.1 deaths per day.
Deaths in middle-age adults:
Deaths among those age 30-59 accounted for 69% of drug-toxicity deaths in the province and 78% were male, the BC Cornoers Service said in a news release this week.
In 2026, 81% of unregulated drug deaths occurred inside in places like private residences, social and supportive housing, SROs, shelters and other locations, and 18% occurred outside in places like vehicles, sidewalks, streets and parks.
The highest number of unregulated drug deaths by health authority in the first two months of 2026 were in the Fraser and Vancouver Coastal health authorities (62 and 74 deaths, respectively), making up 51% of all such deaths. Those are also the most highly populated regions of the province.
Stimulants in over 80% of cases:
Stimulants are the most common substances detected in expedited toxicological testing in 2026. Over 80% of decedents who underwent expedited testing were found to have stimulants (83%), followed by fentanyl or its analogues (80%), and benzodiazepines (36%).
Smoking continues to be the most common mode of consumption (71%), followed by nasal insufflation (9%), injection (9%) and oral (2%).
The unregulated toxic drugs dashboard (BC Centre for Disease Control) has now been updated to include xylazine and medetomidine detection on the “Drugs Detected” page.
Use of toxic drugs — if not leading to death — often leaves people with permanent brain injury which devastates individual lives and families and adds a further load to the health-care system (treatment, long-term care).
Government statements:
Minister of Health Josie Osborne and Provincial Health Officer Dr. Bonnie Henry have issued statements on April 13 in marking the 10th anniversary of the toxic-drug crisis being declared a public-health emergency.
On Monday morning they also held a roundtable discussion about the 10th anniversary of the toxic-drug public-health emergency.
Health Minister:
Minister Osborne’s statement leads with highlighting “increasingly unpredictable and highly toxic street drugs” but she acknowledges some of the surrounding circumstances of drug-related deaths:
“Substance use often begins with experiences such as trauma, mental- and physical-health challenges, poverty, stigma and barriers to safe and stable supports. No one sets out intending to become addicted. That is why we continue to fight stigma and break down barriers to keep people alive and ensure they can access the help they need,” said Osborne.
See full statement from Minister Osborne.
Provincial Health Officer:
Dr Bonnie Henry leads with a similar comment: “Over the years, the increasingly toxic and unpredictable street-drug supply has turned an already serious situation into something far more dangerous, putting people at extreme and increased risk.”
She goes on to itemize some of the circumstantial factors:
“The emergency has been exacerbated by various factors, including the COVID-19 pandemic, gaps in the health-care system, housing instability and homelessness, poverty, the impacts of colonialism and racism, criminalization and stigma, as well as other determinants of health,” said Dr Henry in the April 13 statement.
“People working in the trades, men and Indigenous people continue to experience a disproportionate number of overdoses and deaths, and many of those we are losing do not have substance-use disorders, underscoring how unpredictable and dangerous the drug supply has become,” said Dr Henry.
“This crisis remains a public-health emergency that demands a continued response rooted in compassion, respect and evidence,” she said.
See full statement from Dr Henry.
Timeline since 2016:
This week the government released a timeline of this journeyed drug crisis that is a health emergency, starting with the declaration of the health emergency in 2016 through to 2026 where the current focus is on supports within the health-care system.
Some timeline excerpts:
- In 2016, Dr. Perry Kendall, B.C.’s public health officer at the time, declared a public-health emergency as overdose deaths surged due to a toxic-drug supply.
- In 2017, the Province committed $322 million over three years for overdose prevention, treatment and recovery, and public awareness.
- In 2018, the Province and the Government of Canada funded approximately $34 million from the Emergency Treatment Fund to improve treatment and care, and to contribute to improved health and social outcomes for people living with opioid-use disorder.
- Also in 2018, the BC Coroners Service Death Review Panel report: A Review of Illicit Drug Toxicity Deaths, was released.
- In 2019, the Province implemented a distributed-drug sample collection model and health authorities gradually expanded their support of drug checking.
- In 2020, the Province rolled out prescribed safer-supply programs, providing regulated alternatives to unregulated drugs for people at high risk of overdose. As of 2026, more than 17,000 people have accessed the program.
- In 2021, the Province provided Canadian Mental Health Association (CMHA) $13.5 million to fund 105 treatment and recovery beds in the province. The Province provided more than $50 million over three years to support 123 new youth substance-use (YSU) beds and enhance provincially accessible specialized beds. The Foundry BC mobile app was launched to enable access to services from anywhere in the province, particularly for youth who face barriers to accessing in-person care
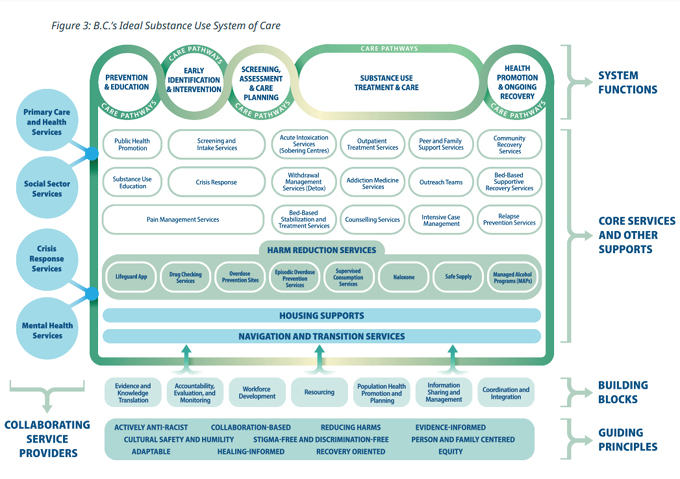
- In 2022, the Ministry of Mental Health and Addictions released the Adult Substance Use System of Care Framework, a technical policy document that articulates an overarching vision for a substance-use system of care
- In 2023, the Ministry of Health supported the BC College of Nurses and Midwives to establish a new designation of certified practice for opioid-use disorder for registered nurses and registered psychiatric nurses.
- In 2024, the Province announced a short-term pilot project to distribute nasal naloxone kits through the BCCDC THN program and now in 2026 has announced a $50-million investment to expand access to nasal naloxone through the BCCDC naloxone program.
- In 2024, then Minister of Public Safety and Solicitor General Mike Farnworth acknowledged the criminal element, saying: “As we continue to go after the gangs and organized criminals who are making and trafficking toxic drugs, we’re taking action now to make it illegal to use drugs in public spaces, and to expand access to treatment to help people who need it most.” [See April 26, 2024 news release]
- As of 2025, the Province provided more than $500 million to support and sustain addictions treatment and recovery programs established through previous budgets.
- As of April 2026, the Province added more than 829 publicly funded substance-use treatment and recovery beds in the province, for a total of 3,875.
- To date (since 2022), complex care housing services are in place for more than 600 people, with government and BC Housing working to build new housing for people living with addictions issues.
See full timeline in the BC Health news release (April 13, 2026).
BC Greens Commentary:
“The government declared this an emergency—it’s time they acted like it,” say the BC Greens in a statement this week.
The BC Greens are calling for expanded harm reduction measures and says “every death in this crisis is a policy choice” where they say the government is not guided by evidence but by policy.
The BC Greens say there should be an expansion of “voluntary, community-based treatment, providing regulated pharmaceutical alternatives, and establishing consistent, evidence-based standards of care across the province”.
The BC Greens point out a statement by B.C.’s Human Rights Commissioner, Kasari Govender: This is a human rights crisis—driven by toxic supply and structural inequality—that disproportionately harms marginalized communities.

Working around the edges:
Perhaps the BC government is recognizing root causes as including insufficient employment ad/or education leading to despair, socioeconomic struggle, a sense of social exclusion and possibly homelessness.
But in announcing that their the BC government’s three-year decriminalization pilot has concluded and will not be renewed has been challenged by both Dr Henry and the BC Greens. Clearly it makes no sense to put criminal blame on people who possess small amounts for personal use, regardless of how dangerous or unhelpful it is to use drugs. That just ties up the criminal system and adds to problems of record for anyone accused of drug possession, rather than getting to the root cause of the drug use and helping people find alternative lifestyles.
Federal Conservatives have been weighing in. Opposition Party’s Health Critic Dan Mazier, MP (Riding Mountain) does not support supplying drugs to people but reorienting resources to focus on getting people off drugs. In the meantime, he has brought forward Private Members’ Bill Bill C-272 which aims to ban supervised drug consumption and injection sites from operating within 500 metres of schools, daycares and playgrounds. This would be at the federal level to set the tone for all provinces.
As of April 2024, BC already has legislation to keep drug use away from schools, parks and playgrounds — something the BC Conservatives (BC Liberals/United at the time) pushed for.
===== RELATED:
- Fentanyl through smoking contributes to 75% of drug-related deaths in BC (March 13, 2026)
- BC Coroner’s report on reducing suicide opens discussion on societal supports (October 15, 2025)
- BC Greens: schools need more funding for youth drug education & supports (September 24, 2024)
- BC overdose crisis continues at six deaths per day (August 31, 2023)
- Addressing root causes of toxic drug public health emergency (April 14, 2023)
NEWS SECTIONS: HEALTH | MENTAL HEALTH & ADDICTIONS