Monday December 28, 2020 | VANCOUVER ISLAND, BC
by Mary P Brooke, B.Sc., editor | Island Social Trends
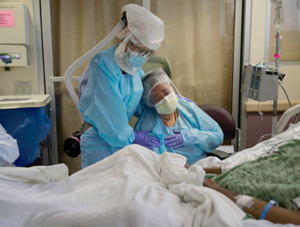
The COVID-19 pandemic has turned 2020 into a long hard slog for all frontline health-care professionals. We hear of the impact on long-term care, but not as much about nurses so far.
Particularly in the context of the surgical renewal as instituted by the BC Ministry of Health since May (to catch up for the thousands of cancelled surgeries and procedures in the first wave of the pandemic this spring — an action recommended by public health so that hospital capacity would not be overloaded), nurses have been working long hard hours.
Not only is the well-being of nurses of concern (think of the impact of continued exposure to crisis and death, including dealing with the families), but the variable level of care that patients might receive in the context of exhausted personnel, regardless of professional standards and good intentions.

On Christmas Eve it became known that COVID-19 had been found in patients a few days earlier at Vancouver General Hospital (see VGH outbreak list). COVID-19 is a virus and it spreads wherever and however it can; but showing up as an outbreak in BC’s largest hospital only underscores the importance of all systems being at top efficiency during the ongoing pandemic.
In particular, the well-being and availability of full staffing of critical care nurses on the COVID frontlines is most certainly needed at optimum levels in order to maintain the current success rate in intensive care units (ICUs) in BC.
Surgical renewal impact:
A best-case scenario was put forward by Health Minister Adrian Dix on May 7 when he called for the surgical renewal — including that health-care professionals (including doctors, nurses, technicians and everyone else involved in the delivery of acute care in hospitals) would commit to and perform at their very best. And no one doubts that in terms of the professionalism of health-care workers in BC. A further update was given by Dix on September 1, including higher surgical counts year-to-date.

However, people and systems that are worked at full capacity for a long while will begin to show wear and tear. That’s just the natural way of things — every person and every system requires pauses and maintenance from time to time.
So far, only the ‘push’ has been articulated by BC Health, with relatively little to no mention of the maintenance and management of the strident push that the fight against COVID-19 — like a war movement — has been thrust upon the BC health-care system.
BC Nurses Union speaks up:
BC Nurses Union (BCNU) President Christine Sorensen in her year-end statement to BCNU members says that nurses are stepping up to help reduce the surgical backlog created when operating rooms across the province were shut down this spring. But she points out: “The health ministry’s surgical renewal plan presumes all operating room (OR) nurses in BC can work full time and that all new grads hired this year are competent enough to work in the OR.”

Indeed, from the start of the pandemic it has been presumed that all needed personnel have been available and in place. Boasting that all new nursing grads would be offered positions (including in hospitals) was an enthusiastic stance in April, but perhaps didn’t count on the skill-set challenge that Sorensen mentions, or indeed that all (or even most) grads would want to sign-on to the first days, weeks and months of their new careers during a global pandemic.
“All of these measures press on the capacity of the system and nurses’ ability to cope while we struggle to get through a difficult winter as COVID cases increase,” continues Sorensen. “They also speak to the need for a provincial health human resources plan specific to nursing if we want to avoid the downward spiral of exhaustion, depression, burnout and reduced retention rates that inaction will inevitably bring,” she wrote.
Island Social Trends has been waiting to have questions around this issue answered by Minister Dix during media teleconferences, and the same thread of question was submitted by email to BC Health communications before Christmas. We will report further on this as more insights are developed.
Vaccination to frontline health-care:
Meanwhile, the guidance of the Provincial Health Officer and the policy of BC Health is to provide the new COVID-19 vaccination doses first to frontline health-care workers (some of those in long-term care). Certainly that is a stance shared by all.
The stated priority from there is to vaccinate people in remote and Indigenous communities (for which the more-easily-shipped Moderna vaccine product is targeted). Then the vaccination program will focus on people over the age of 80 years, then over the age of 70 years.
There is no definitive public health policy statement in BC yet, as to what happens from there in terms of economic sectors or age groups, though teachers in BC have been asking for attention to their interest in being vaccinated given their frontline exposure to children in schools.
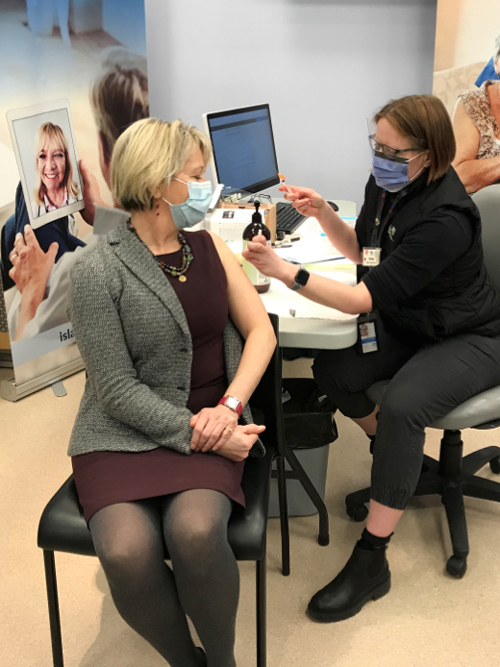
As part of promoting the safety of the new mRNA-type vaccines from Pfizer-BioNTech, on December 22 Provincial Health Officer Dr Bonnie Henry and Island Health Chief Medical Health Officer Dr Richard Stanwick received their first dose of the vaccine in Victoria.
Reportedly on this Monday evening at the tail-end of the Christmas long-weekend, some administrators have been receiving vaccinations ahead of frontline health care workers, according to BCNU President Sorensen.